Ayurveda the “science of life”, usually rendered simply ayurveda in English) or ayurvedic medicine is a system of traditional medicine native to the Indian subcontinent and practiced in other parts of the world as a form of alternative medicine.
In Sanskrit, the word ayurveda consists of the words ayus, meaning “life”, and veda, meaning “related to knowledge” or “science”.
Evolving throughout its history, ayurveda remains an influential system of medicine in South Asia. The earliest literature of ayurveda appeared during the Vedic period in India.
The Sushruta Samhita and the Charaka Samhita were influential works on traditional medicine during this era. Ayurvedic practitioners, called “Ayurvedacharyas”, have also identified a number of medicinal preparations and surgical procedures for curing various ailments and diseases.
Ayurveda is considered to be a form of complementary and alternative medicine (CAM) in the western world, where several of its methods, such as the use of herbs, massage, and yoga, are applied on their own as a form of CAM treatment.
Ayurveda is grounded in a metaphysics of the “five great elements”( earth, water, fire, air and ether)—all of which compose the Universe, including the human body.
Chyle or plasma (called rasa dhatu), blood (rakta dhatu), flesh (mamsa dhatu), fat (medha dhatu), bone (asthi dhatu), marrow (majja dhatu), and semen or female reproductive tissue (shukra dhatu) are held to be the seven primary constituent elements of the body.
Ayurveda deals elaborately with measures of healthful living during the entire span of life and its various phases. Ayurveda stresses a balance of three elemental energies or humors: vata (air & space – “wind”), pitta (fire & water – “bile”) and kapha (water & earth – “phlegm”).
According to ayurveda, these three regulatory principles— Doshas (literally that which deteriorates – the elements)—are important for health, because when they are in balanced state, the body is healthy, and when imbalanced, the body has diseases.
Ayurveda holds that each human possesses a unique combination of Doshas. In ayurveda, the human body perceives attributes of experiences as 20 Guna (meaning qualities). Surgery and surgical instruments are employed.
It is believed that building a healthy metabolic system, attaining good digestion and proper excretion leads to vitality. Ayurveda also focuses on exercise, yoga, meditation, and massage.
Thus, body, mind, and spirit/consciousness need to be addressed both individually and in unison for health to ensue. As Robert Svoboda attempts to summarize the three major paths of the Vedic knowledge, he exclaims:
“Because every embodied individual is composed of a body, a mind and a spirit, the ancient Rishis of India who developed the Science of Life organized their wisdom into three bodies of knowledge: Ayurveda, which deals mainly with the physical body; Yoga, which deals mainly with spirit; and Tantra, which is mainly concerned with the mind.
The philosophy of all three is identical; their manifestations differ because of their differing emphases. Ayurveda is most concerned with the physical basis of life, concentrating on its harmony of mind and spirit.
Yoga controls body and mind to enable them to harmonize with spirit, and Tantra seeks to use the mind to balance the demands of body and spirit.”The practice of Panchakarma is believed to eliminate toxic elements from the body.
Eight Disciplines Of Ayurveda Treatment Called Ashtangas Are Given Below:
Internal medicine (Kaaya-chikitsa)
• Paediatrics (Kaumarabhrtyam)
• Surgery (Shalya-chikitsa)Treatment of diseases above the clavicle (Salakyam) • Demonic possession (Bhuta vidya): Bhuta vidya has been called psychiatry.[ Toxicology (Agadatantram) • Prevention diseases and improving immunity and rejuvenation (rasayana) • Aphrodisiacs and improving health of progeny (Vajikaranam) Dhanvantaris Dhanvantari is said to be an avatar of Vishnu from the Hindu tradition, and god of ayurvedic medicine. Dhanvantari was an early Indian medical practitioner and one of the world’s first surgeons.
Based on Vedic traditions, he is regarded as the source of ayurveda.He perfected many herbal based cures and natural remedies and was credited with the discovery of the antiseptic properties of turmeric and the preservative properties of salt which he incorporated in his cures.
“I the Lord Dhanvantri brought this healing science on earth from heaven.”- Quote of Dhanvantri himself in the literature concerned Practices
Several philosophers in India combined religion and traditional medicine—notable examples being that of Hinduism and ayurveda.
Shown in the image is the philosopher Nagarjuna—known chiefly for his doctrine of the Madhyatmika (middle path)—who wrote medical works The Hundred Prescriptions and The Precious Collection, among others.
Hinduism and Buddhism have been an influence on the development of many of ayurveda’s central ideas — particularly its fascination with balance, known in Buddhism as Madhyatmika .
Balance is emphasized; suppressing natural urges is seen to be unhealthy, and doing so may almost certainly lead to illness. To stay within the limits of reasonable balance and measure is stressed upon.
Ayurveda places an emphasis on moderation in food intake, sleep, sexual intercourse, and the intake of medicine. Ayurveda incorporates an entire system of dietary recommendations.
Chopra (2003) writes on this topic: “Ayurvedic dietetics comprises a host of recommendations, ranging from preparation and consumption of food, to healthy routines for day and night, sexual life, and rules for ethical conduct. In contrast to contemporary practitioners of New Age Ayurveda, older Ayurvedic authors tended to be religiously neutral.
Even Buddhist authors refrained from trying to convert the patient to follow their particular religious ways.”
For diagnosis the patient is to be questioned and all five senses are to be employed. The Charaka Samhita recommends a tenfold examination of the patient.
The qualities to be judged are: constitution, abnormality, essence, stability, body measurements, diet suitability, psychic strength, digestive capacity, physical fitness and age.Hearing is used to observe the condition of breathing and speech.
The study of the vital pressure points or marma is of special importance.
It is the trauma science described in ayurveda. There are 107 different spots described and located on the body surface which produce different signs and symptoms. With respect to the underlying anatomical structures, the symptoms vary according to blunt or penetrating trauma.
The severity of the symptoms and signs also depend on whether the injury is exactly on the marma point or slightly around it. These signs and symptoms are described by Sushruta and Wagbhatta.
Chopra (2003) identifies five influential criteria for diagnosis: ‘origin of the disease, prodrominal (precursory) symptoms, typical symptoms of the fully developed disease, observing the effect of therapeutic procedures, and the pathological process’.
Hygiene — also a component of religious virtue to many Indians — is a strong belief. Hygienic living involves regular bathing, cleansing of teeth, skin care, and eye washing. Occasional anointing of the body with oil is also prescribed.
Oils such as sesame and sunflower oil are extensively used in ayurvedic medicine. Studies show that both these oils contain substantial amount of linoleate in triglyceride form. Oils rich in linoleic acid may have antineoplastic properties.
Hundreds of vegetable drugs are used in ayurvedic medicine—including cardamom and cinnamon.Ayurveda stresses the use of vegetable drugs. Fats are used both for consumption and for external use.
Hundreds of vegetable drugs are employed, including cardamom and cinnamon. Some animal products may also be used, for example milk, bones, and gallstones. Minerals, including sulphur, arsenic, lead, copper sulphate and gold are also consumed as prescribed.
This practice of adding minerals to herbal medicine is known as rasa shastra.
In some cases, alcohol is used as a narcotic for the patient undergoing an operation. The advent of Islam introduced opium as a narcotic. Both oil and tar are used to stop bleeding.
Traumatic bleeding is said to be stopped by four different methods ligation of the blood vessel; cauterisation by heat; using different herbal or animal preparations locally which facilitate clotting; and different medical preparations which constrict the bleeding or oozing vessels.
Different oils may be used in a number of ways including regular consumption as a part of food, anointing, smearing, head massage, and prescribed application to infected areas.
The proper function of channels (srotas) that transport fluids from one point to another within the body is seen as vital, and the lack of healthy srotas may lead to disease and insanity.
Sushruta identifies that blockages of these channels may lead to rheumatism, epilepsy, paralysis, and convulsions as fluids and channels are diverted from their ideal locations.
Sweating is used as a means to open up the channels and dilute the Doshas causing the blockages and harming a patient.
A number of ways to take steam bathing and other steam related cures are recommended so that toxins are released.
History
Chanting mantras has been a feature of ayurveda since the Atharvaveda, a largely religious text, was compiled.Around 1500 BCE, ayurveda’s fundamental and applied principles got organised and enunciated.
Ayurveda traces its origins to the Vedas, Atharvaveda in particular, and is connected to Hindu religion.
Atharvaveda (one of the four most ancient books of Indian knowledge, wisdom and culture) contains 114 hymns or formulations for the treatment of diseases. Ayurveda originated in and developed from these hymns.
In this sense, ayurveda is considered by some to have divine origin. Indian medicine has a long history, and is one of the oldest organised systems of medicine.
Its earliest concepts are set out in the sacred writings called the Vedas, especially in the metrical passages of the Atharvaveda, which may possibly date as far back as the 2nd millennium BC.
According to a later writer, the system of medicine was received by a man named Dhanvantari from Brahma, and Dhanvantari was deified as the god of medicine.
In later times his status was gradually reduced, until he was credited with having been an earthly king.
The Sushruta Samhita of Sushruta appeared during the 1st millennium BCE. Dwivedi & Dwivedi (2007) – on the work of the surgeon Sushruta – write.The main vehicle of the transmission of knowledge during that period was by oral method.
The language used was Sanskrit — the vedic language of that period (2000–500 BCE). The most authentic compilation of his teachings and work is presently available in a treatise called Sushruta Samhita.
This contains 184 chapters and description of 1,120 illnesses, 700 medicinal plants, 64 preparations from mineral sources and 57 preparations based on animal sources.”
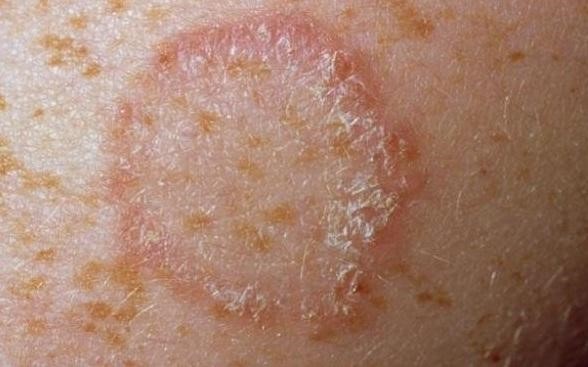
Underwood & Rhodes (2008) hold that this early phase of traditional Indian medicine identified ‘fever (takman), cough, consumption, diarrhea, dropsy, abscesses, seizures, tumours, and skin diseases (including leprosy)’.
Treatment of complex ailments, including angina pectoris, diabetes, hypertension, and stones, also ensued during this period.
Plastic surgery, cataract surgery, puncturing to release fluids in the abdomen, extraction of foreign elements, treatment of anal fistulas, treating fractures, amputations, cesarean sections, and stitching of wounds were known.
The use of herbs and surgical instruments became widespread. The Charaka Samhita text is arguably the principal classic reference. It gives emphasis to the triune nature of each person: body care, mental regulation, and spiritual/consciousness refinement.
Cataract surgery was known to the physician Sushruta in the first millennium BCE, and was performed with a special tool called the jabamukhi salaka, a curved needle used to loosen the lens and push the cataract out of the field of vision.
The eye would later be soaked with warm butter and then bandaged.
Other early works of ayurveda include the Charaka Samhita, attributed to Charaka. The earliest surviving excavated written material which contains the works of Sushruta is the Bower Manuscript, dated to the 4th century CE.
The Bower manuscript quotes directly from Sushruta and is of special interest to historians due to the presence of Indian medicine and its concepts in Central Asia.
Vagbhata, the son of a senior doctor by the name of Simhagupta, also compiled his works on traditional medicine.
Early ayurveda had a school of physicians and a school of surgeons. Tradition holds that the text Agnivesh tantra, written by the sage Agnivesh, a student of the sage Bharadwaja, influenced the writings of ayurveda.
The Chinese pilgrim Fa Hsien (ca. 337–422 CE) wrote about the health care system of the Gupta empire (320–550) and described the institutional approach of Indian medicine, also visible in the works of Charaka, who mentions a clinic and how it should be equipped.
Madhava (fl. 700), Sarngadhara (fl. 1300), and Bhavamisra (fl. 1500) compiled works on Indian medicine. The medical works of both Sushruta and Charaka were translated into the Arabic language during the Abbasid Caliphate (ca. 750).
These Arabic works made their way into Europe via intermediaries. In Italy, the Branca family of Sicily and Gaspare Tagliacozzi (Bologna) became familiar with the techniques of Sushruta.
British physicians traveled to India to see rhinoplasty being performed by native methods. Reports on Indian rhinoplasty were published in the Gentleman’s Magazine in 1794. Joseph Constantine Carpue spent 20 years in India studying local plastic surgery methods.
Carpue was able to perform the first major surgery in the western world in 1815. Instruments described in the Sushruta Samhita were further modified in the Western World.
Inside India
In 1970, the Indian Medical Central Council Act which aims to standardize qualifications for ayurveda and provide accredited institutions for its study and research was passed by the Parliament of India.
In India, over 100 colleges offer degrees in traditional ayurvedic medicine.
The Indian government supports research and teaching in ayurveda through many channels at both the national and state levels, and helps institutionalize traditional medicine so that it can be studied in major towns and cities.
The state-sponsored Central Council for Research in Ayurveda and Siddha (CCRAS) is the premier institution for promotion of traditional medicine in India.
The studies conducted by this institution encompass clinical, drug, literary, and family welfare research.The Bachelor of Ayurveda, Medicine & Surgery (BAMS) degree is the basic five-and-a-half year course of graduation.
It includes eighteen different subjects comprising courses on anatomy with cadaver dissections, physiology, pharmacology, pathology, modern clinical medicine & clinical surgery, paediatrics, along with subjects on ayurveda like Charaka Samhita, history and evolution of ayurveda, identification and usage of herbs (dravyaguna), and ayurvedic philosophy in diagnostics and treatment.
Practicing graduates are governed under different state laws Many clinics in urban and rural areas are run by professionals who qualify from these institutes.
Mukherjee & Wahile cite World Health Organization statistics to demonstrate the popularity of traditional medicine as the primary system of health care.
In Sri Lanka, the number of traditional ayurveda practitioners is greater than trained modern medicine professionals.
Dr. Partap Chauhan established the world’s first online ayurvedic clinic, Ayurvedic.org, in India in 1995.
A pioneer of online ayurvedic medicine, Chauhan is also credited with setting up the world’s first ayurvedic telemedicine center in Faridabad, Haryana. Dr K. P.
Manikandan established world’s first ISO-certified ayurveda pediatric hospital in Mezhathur, Kerala, under the name CNS Ayurveda Chikitsalayam.
Outside India
Academic institutions related to traditional medicine in India have contributed to ayurveda’s international visibility. Kurup (2003) comments on the role of Gujarat Ayurved University: “The Gujarat Ayurved University has signed a Memorandum of Understanding (MoU) with nine ayurvedic institutes functioning in Japan, Australia, the Netherlands, Italy, Argentina, and Germany to coordinate and facilitate the globalization of ayurveda through academic collaboration.
Earlier, Medical (Ayu) Institute of Russia had signed the MoU with the government of India, in which Gujarat Ayurved University is also one of the implementing authorities.”
Ayurveda gained recognition in the Western world as medical scholars, notably Frank John Ninivaggi MD of Yale University School of Medicine, researched and outlined its various postulates in one major textbook suitable to Western academic science.
In the United States of America, the National Center for Complementary and Alternative Medicine (NCCAM) of the [[National Institutes of Health expends some of its $123 million annual budget on ayurvedic medicine research.
In addition, the National Institute of ayurvedic Medicine, established by Dr. Scott Gerson, is an example of an ayurveda research institute.
Gerson has published part of his work on the antifungal activities of certain ayurvedic plants in academic journals. The postulates and history of ayurveda have also been outlined by foreign scholars such as Dominik Wujastyk in the United Kingdom.
Questionable practices in research involving financial gains have resulted in the questioning of some of the research and cases such as the Maharishi Vedic Approach to health have involved litigations.
Journals
A variety of peer reviewed journals focus on the topic of ayurvedic medicine, including the Theoretical and Experimental Journal of Ayurveda and Siddha (TEJAS; published between 1981 and 2008 as Ancient Science of Life) the Journal of Research & Education in Indian Medicine (JREIM), AYU (published quarterly) and The International Journal for Ayurveda Research (IJAR, published quarterly). None of the journals are Pub Med indexed.
Patents
In December 1993, the University of Mississippi Medical Centre had a patent issued to them by United States Patent and Trademark Office on the use of turmeric for healing.
The patent was contested by India’s industrial research organization, Council for Scientific and Industrial Research (CSIR), on the grounds that traditional ayurvedic practitioners were already aware of the healing properties of the substance for centuries, and that this prior art made the patient a case of biopiracy.
The Government of India had become involved in promoting traditional medicine by 1997. Sharma & Bodeker report on the various government activities in relation to ayurveda:
“In India the government became involved in traditional drug production when the Central Drug Research Institute patented two new drugs from ancient ayurvedic formulas.
One, a mixture of black pepper, long pepper, and ginger, allows for the dosage of the antibiotic rifampicin to be halved in the treatment of tuberculosis and other mycobacterial infections. The other is a memory tonic produced from the traditional plant called brahmi.
Overseas patenting of turmeric and products of the neem tree caused controversy in India and other nations.
In August the U.S. Patent and Trademark Office cancelled a U.S. patent on the wound-healing properties of turmeric when the Indian government proved that records had existed for this use for centuries.” Scientific evidence
Chemical Structure Of Curcumin Used In Ayurvedic Medicine. Shown Here In Its Ketone Form.
Research suggests that Terminalia arjuna is useful in alleviating the pain of angina pectoris and in treating heart failure and coronary artery disease. T. arjuna may also be useful in treating hypercholesterolemia.
As a traditional medicine, many ayurveda products have not been tested in rigorous scientific studies and clinical trials.
In India, research in ayurveda is largely undertaken by the statutory body of the Central Government, the Central Council for Research in Ayurveda and Siddha (CCRAS), through a national network of research institutes.
A systematic review of ayurveda treatments for rheumatoid arthritis concluded that there was insufficient evidence, as most of the trials were not done properly, and the one high-quality trial showed no benefits.
A review of ayurveda and cardiovascular disease concluded that while the herbal evidence is not yet convincing, the spices are appropriate, some herbs are promising, and yoga is also a promising complementary treatment.
Some ayurvedic products, mainly herbs used for phytotherapy, have been tested with promising results. Turmeric and its derivative curcumin appears to have beneficial properties Tinspora cordifolia has been tested.
Among the medhya rasayanas (intellect rejuvenation), two varieties of Salvia have been tested in small trials; one trial provided evidence that Salvia lavandulifolia (Spanish sage) may improve word recall in young adults and another provided evidence that Salvia officinalis (Common sage) may improve symptoms in Alzheimer’s patients.
In some cases, ayurvedic medicine may provide clues to therapeutic compounds. For example, derivatives of snake venom have various therapeutic properties.
Many plants used as rasayana(rejuvenation) medications are potent antioxidants Neem appears to have beneficial pharmacological properties Azadirachta indica—believed to have immunopotentiating abilities and used often as an anti-infective—has been found to enhance the production of IL-2 and increase immunity in human volunteers by boosting lymphocyte and T-cell count in three weeks.
Black pepper and long pepper are combined with ginger to form the traditional trikatu mixture in ayurveda. This mixture increases appetite, promotes the secretion of digestive juices, and cures certain gastric disorders, particularly achlorhydria and hypochlorhydria.
Mitra & Rangesh (2003) hold that cardamom and cinnamon stimulate digestive enzymes that break down polymeric macromolecules in the human body.
Research suggests that T. arjuna is useful in alleviating the of angina pectoris and in treating heart failure and coronary artery disease. T. arjuna may also be useful in treating hypercholesterolemia.
Richard Dawkins has a critique of the use of ayurveda in the West.
Safety
Major safety concerns include adulteration of herbal medicines with toxic metals, and intrinsic toxicity of herbal medications.
Some traditional ayurvedic treatments use toxic metals, herbs, and minerals as part of their remedies. rasa shastra, the practice of adding metals, minerals or gems to herbs, increases the likelihood of toxic heavy metals such as lead, mercury and arsenic in the remedy.
There is evidence that using some ayurvedic medicines, especially those involving herbs, metals, minerals, or other materials involves potentially serious risks, including toxicity.
Adverse reactions to herbs due their pharmacology are described in traditional ayurvedic texts, but ayurvedic practitioners are reluctant to admit that herbs could be toxic and the reliable information on herbal toxicity is not readily available.
A 2004 study found such toxic metals in 20% of ayurvedic preparations that were made in South Asia for sale around Boston and extrapolated the data to the United States more broadly.
It concluded that excess consumption of these products could cause health risks.
A 2008 study of more than 230 products found that approximately 20% of remedies (and 40% of rasa shastra medicines) purchased over the Internet from both US and Indian suppliers contained lead, mercury or arsenic.
Traditionally the toxicity of these materials are believed to be reduced through purification processes such as samskaras or sadhanas (for metals), which is similar to the Chinese pao zhi, although the ayurvedic technique is more complex and may involve prayers as well as physical pharmacy techniques.
One medical journal reported: “Crude aconite is an extremely lethal substance, yet ayurveda looks upon it as a therapeutic entity. Crude aconite is always processed, i.e. it undergoes ‘samskaras’ before being utilised in the Ayurvedic formulations.
This study was undertaken in mice, to ascertain whether “processed” aconite is less toxic as compared to the crude or unprocessed one.
It was seen that crude aconite was significantly toxic to mice (100% mortality at a dose of 2.6 mg/mouse) whereas the fully processed aconite was absolutely non-toxic (no mortality at a dose even 8 times as high as that of crude aconite).
Further, all the steps in the processing were essential for complete detoxification.”Rigorous evidence that the metals may be rendered nontoxic is not available, and case reports describe adverse effects of these metals.
Following concerns about metal toxicity, the Government of India ruled that ayurvedic products must specify their metallic content directly on the labels of the product the harmful effects of the samples is attributed in part to the adulterated raw material and lack of workers trained in traditional medicine.
In a letter to the Indian Academy of Sciences, director of the Interdisciplinary School of Health Sciences, University of Pune Patwardhan Bhushan stated that the metal adulteration is due to contamination and carelessness during the much faster modern manufacturing processes, and does not occur with traditional methods of preparation.
Publication of the levels of contamination found in the products has resulted in some decline of ayurveda in India and abroad.