Have you ever wondered why those extra pounds that came off so easily when you were younger are just not so easy to shed now? Calorie counting is tough and leaves you feeling so guilty, especially when you look at yourself in the mirror, or worse on the scales!
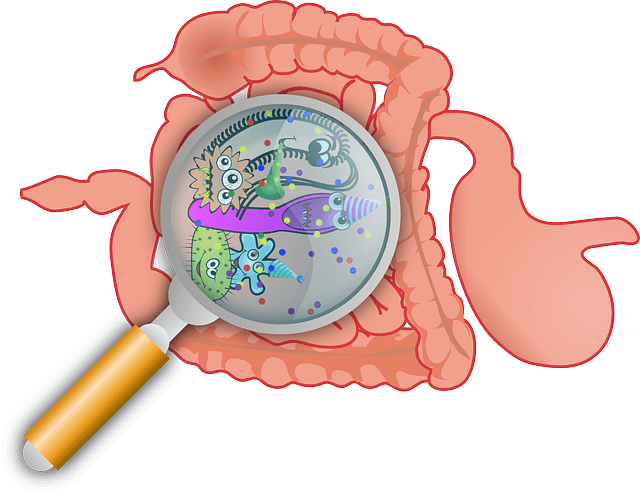
The idea that the health of our GUT flora might influence our overall metabolism and therefore our weight, is relatively new.
The GUT flora plays a crucial role in feeding us because they help in breaking down the food we eat into small “bite sizes”, not visible to the naked eye, so that our body is able to absorb it.
If it were not for these “good guys” we would have expelled all this material, causing our bodies to feel starved, which would have lead our bodies to hold on to every kilojoule of energy, in pursuit of preserving life.
A growing body of evidence is suggesting that naturally occurring bacteria and other microbes in the body, and possibly even viruses, can influence weight in ways that scientists are only just beginning to understand.
Numerous studies are underway looking at the role of intestinal organisms in obesity, with a focus on how they extract energy from food and how this affects weight gain or loss.
Insights gained from this research could identify people predisposed to obesity and possibly help clinicians create targeted weight-loss treatments for them.
The specific composition of microbes in the intestines also might help predict the best candidates for weight-loss surgery, which doesn’t work for everyone.
The Obesity – Bacteria Link
Researchers speculate that people are more likely to gain weight when gut bacteria are more efficient at breaking down food, enabling the body to absorb more calories. They theorize that less-efficient bacteria allow food to pass more quickly through the intestines.
“If you want to stay lean, you’ll want bacteria that are not very efficient,” says Claire Fraser, a professor of medicine and microbiology and immunology at the University Of Maryland School Of Medicine.
“If we each eat a bowl of cereal and your bacteria are better than mine at breaking it down, you’ll get 95 calories, while I’ll only get 70, and the rest will pass through. You’re the one who’s going to gain weight.”
The food one eats contributes to the composition of the bacterial communities in the gut.
For example, Fraser says, “high-fat, low-fibre diets have been associated with different bacteria in the gut than low-fat, high-fibre diets,” which may play a role in who develops obesity. “It may be a vicious cycle but one we can interrupt by altering our dietary habits.”
Recent studies by Stanley Hazen of the Cleveland Clinic, for example, have found that gastrointestinal bacteria “burp” out a chemical called TMAO (for trimethylamine N-oxide) after people consume red meat or eggs.
TMAO increases the risk of heart attack and stroke, which may help explain why eating those foods increases the danger of heart disease more than following a vegan or vegetarian diet.
“Chubby” Bacteria, Gut Bugs, Stress & Inflammation?
When the body has been subjected to stress, and this may be as little as twenty four hours, the “unhealthy” microbes start to overpower the “good ones”.
The unhealthy bacteria are……. more fat storing in nature than fat burning, understandable from our innate survival instinct.
In an obese individual, we see an overgrowth of these fat storing, “chubby” bacteria.
These “chubby” bacteria extract even the last ounce of energy from the food consumed, which causes the individual to pile on weight, even if they didn’t eat more than others.
It could be that their gut flora is extracting more energy from the food they eat.
Studies carried out on obese subjects reveal that they have less overall diversity of the gut microbial flora and primarily the “chubby” bacteria prevail.
Simply put, an overweight person is more likely to harbour a gut flora that’s imbalanced and a digestive system that is “weak”.
More specifically, there is damage to the “biofilm”, a flimsy mucus layer forming a protective coating over the inner lining of our gut.
Damage to this layer causes the gut to become “leaky” setting up inflammation, which is now being proposed as another major cause of obesity and its related problems of diabetes and metabolic syndrome.
It is an interesting observation that obese individuals with metabolic syndrome, diabetes and high blood lipids, also have a high level of infection markers in their bloods too.
The levels are not so high to warrant active treatment, however the levels are elevated enough to fall in the category of “sub clinical“ infection. This inflammation is setup by the “leaky gut”, caused by an unhealthy gut flora causing damage to the protective biofilm.
The leaky gut causes far too much of the food particles and other bacteria to escape through the tight protective wall, leading to ongoing “subclinical infection”.
From an evolutionary point of view any infection is a form of stress and in such a situation, the body elects to conserve every ounce of energy. This is due to being in a state of “perceived stress” due to the subclinical infection.
Research has also identified certain species of gut bacteria that were found at different concentrations in obese individuals who had, or didn’t have, metabolic syndrome.
Weight Loss Surgery & Microbes
An article on weight loss is never complete without mention of Weight loss surgery (especially when the author is a Bariatric surgeon!)The discovery of the role that microbes have to play in making weight loss surgery work has been extremely fascinating.
It is well acknowledged that weight loss surgery is not for everyone, but there are people who are in desperate need for something drastic (accepting that surgery is drastic. And the most powerful tool available to us today!)
It would be fascinating to visualise how the gut microbes could influence outcomes after weight loss surgery.
Also the possibility that a stool analysis could predict which individuals could benefit more from weight loss surgery than the others, is mind blowing.
In an article published in the Aug. 4 issue of the journal Cell Metabolism Volume 22, Issue 2, p228–238, 4 August 2015, researchers analysed the gut bacteria of 14 women nearly a decade after they underwent bariatric surgery ( Gastric bypass and Vertical Banded Gastroplasty).
Microbes from the stool samples of women who underwent these procedures were transplanted into specially bred “germ-free” mice that were devoid of any gut bacteria.
Microbes from a separate group of obese women who had not undergone bariatric surgery, were also transplanted into similar mice via the same method.
Women who had undergone gastric bypass surgery, had more significant differences in the composition of their gut bacteria than the women with severe obesity who had not had surgery.
But what was most interesting was, when researchers took the gut microbes from women that had undergone RYGB and transferred it to a germ-free mouse that had never had surgery, the recipient mouse lost weight.
This showed that something about the post-RYGB gut microbiota, not necessarily the surgery itself, could help the mouse slim down.
These results suggest that the gut microbiota may play a direct (and possibly independent) role in the reduction of body fat observed after bariatric surgery. Several strains and brands of probiotics are being investigated to increase the durability of weight loss surgery, which (unfortunately) doesn’t work for everyone.
It would be fair to summarise, that the ecosystem that rests within our gut has immense abilities to shape our health. If we understand and work in “symbiosis” with it, sound health will be ours, otherwise a malady of ailments (including obesity) will drag us to our end!
“IF YOU THINK THE PURSUIT OF GOOD HEALTH IS EXPENSIVE AND TIME CONSUMING, TRY ILLNESS” – Lee Swanson
TIPS: Putting Science Into Practice:
- Calorie Counting is one of the worst ways to achieve long term weight loss.
- A varied wholefood diet focussed at building a healthy, balanced and diverse gut microbiome is the best option for long term success.
- Inflammation, is the basis of obesity and its associated complications of diabetes and metabolic syndrome. The seat of this inflammation is the gut lining.
- The best probiotic is your diet, however, one may need to take support of a commercial probiotic preparation to get started.
- The long term results of weight loss surgery depend on the quality and health of the gut microbiome.
You can find much more information on living a holistic lifestyle in these free magazines and on our YouTube channel.
 Dr Arun Dhir,FRCS,FRACS – Gastro Intestinal Surgeon, Health & Wellness Advocate
Dr Arun Dhir,FRCS,FRACS – Gastro Intestinal Surgeon, Health & Wellness Advocate