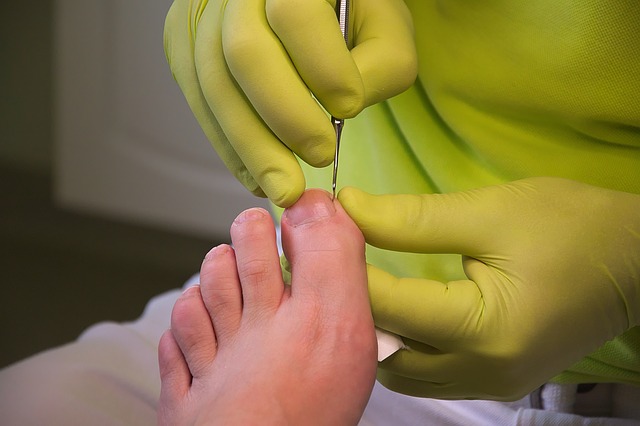
Podiatry is a branch of medicine devoted to the study, diagnosis and treatment of disorders of the foot, ankle and lower leg.
The term “podiatry” came into use first in the early 20th century United States where it now denotes a Doctor of Podiatric Medicine (DPM), also known as a podiatric physician or surgeon who is qualified by their education and training to diagnose and treat conditions affecting the foot, ankle and related structures of the leg.
Within the field of podiatry, practitioners can focus on many different specialty areas, including surgery, sports medicine, biomechanics, geriatrics, pediatrics, orthopedics or primary care.
Podiatry is also practiced in other countries such as Canada, Ireland, the United Kingdom, Malta, Cyprus, South Africa, Australia and New Zealand.
In many English-speaking countries, the older title of “chiropodist” may still be used by some clinicians but is gradually falling out of use.
In many non-English-speaking countries of Europe, the title used instead of podiatrist may be “podologist” or” “Podólogo”. The level and scope of practice may vary in these countries as compared in the US.
History
The professional care of feet was in existence in ancient Egypt as evidenced by bas-relief carvings at the entrance to Ankmahor’s tomb dating from about 2400 BC where work on hands and feet is depicted.
Corns and calluses were described by Hippocrates who recognised the need to physically reduce hard skin, followed by removal of the cause. He invented skin scrapers for this purpose and these were the original scalpels.
Aulus Cornelius Celsus, a Roman scientist and philosopher, was probably responsible for giving corns their name.
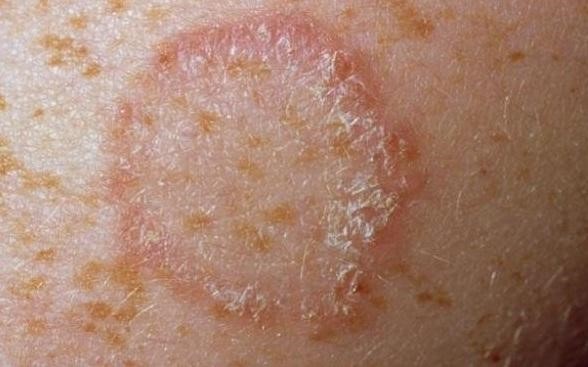
Later Paul of Aegina (AD 615-690) defined a corn as “a white circular body like the head of a nail, forming in all parts of the body, but more especially on the soles of the feet and the toes.
It may be removed in the course of some time by paring away the prominent part of it constantly with a scalpel or rubbing it down with pumice. The same thing can be done with a callus.”
Until the turn of the 20th century, chiropodists—now known as podiatrists—were separate from organized medicine. They were independently licensed physicians who treated the feet, ankles and related leg structures.
Lewis Durlacher was one of the first people to recognize the need for a protected profession. He tried to establish the first association of practitioners in 1854, although it would take another century to come to pass.
There are records of the King of France employing a personal podiatrist, as did Napoleon.
In the United States, President Abraham Lincoln suffered greatly with his feet and chose a chiropodist named Isachar Zacharie, who not only cared for the president’s feet, but also was sent by President Lincoln on confidential missions to confer with leaders of the Confederacy during the U.S. Civil War.
The first society of chiropodists, now known as podiatrists, was established in—and still operates in—New York in 1895 as NYSPMA, with the first school opening in 1911.
One year later the British established a society at the London Foot Hospital and a school was added in 1919. In Australia professional associations appeared from 1924 onwards.
The first American journal appeared in 1907, followed in 1912 by a UK journal. In 1939, the Australians introduced a training centre as well as a professional journal. The number of chiropodists increased markedly after the Great War then again after World War II.
Increased numbers of ex-soldiers needing to be gainfully employed gave chiropody a boost and led to the need for registration in all English speaking countries. The study of the foot (i.e. podology), brought greater knowledge to the practice of foot care or podiatry.
Specific country practices
Australia
In Australia, podiatry is classified as an allied health profession, and is practised by individuals licensed by their representative State Boards of Podiatry.
There are seven registration boards and six teaching centres, with two levels of awards — unclassified bachelors degree and honours level.
In Australia there exist 2 levels of professional accreditation and professional privilege: Podiatrist and Podiatric Surgeon (Surgical Podiatrist in the state of Queensland).
Australian podiatrists are able to practise abroad with their qualifications recognised in some Commonwealth countries.
Registration and regulation
Currently, all podiatrists must be registered with the Podiatrists Registration Board in the state or territory they wish to practise in.
Podiatrists wishing to practise in the Northern Territory (which has no registration board) must be registered in at least one other jurisdiction (eg QLD, SA).
However, as part of proposed reforms to the Australian health system, there are plans to move podiatry (like other registered health professions) to a system of National Registration and Accreditation.
This is likely to occur on the 1st July 2010, and the transition to this major reorganisation of registration and oversight will be facilitated by the Australian & New Zealand Podiatry Accreditation Council (ANZPAC).
It is likely there will be ongoing refinement of national policies relating to the practice of podiatry once this process has been completed.
Education & Training
Australian podiatrists complete an undergraduate degree ranging from 3 to 4 years of education.
The first 2 years of this program are generally focused on various biomedical science subjects including anatomy, medical chemistry, biochemistry, physiology and patient psychology, similar to the medical curriculum.
The following two years will then be spent focusing on podiatry specific areas such as podiatric biomechanics and human gait, podiatric orthopaedics or the non-surgical management of foot abnormalities, pharmacology, general medicine, general pathology, local and general anaesthesia, and surgical techniques such as partial and total nail avulsions, wound debridement, and other cutaneous and electrosurgical procedures.
Australian podiatric surgeons are specialist podiatrists with further training in advanced medicine, advanced pharmacology, and training in foot surgery.
Podiatrists wishing to pursue specialisation in podiatric surgery must meet the requirements for Fellowship with the Australasian College of Podiatric Surgeons.
They first complete a degree of 4 years, which includes 2 years of didactic study and 2 years of clinical experience.
Following this, a masters degree must be completed with focus on biomechanics, medicine, surgery, general surgery, advanced pharmacology, advanced medical imaging and clinical pathology.
They then qualify for the status of Registrar with the Australasian College of Podiatric Surgeons. Following surgical training with a podiatric surgeon (3–5 years), rotations within other medical and surgeons’ disciplines, overseas clinical rotations, and passing oral and written exams, Registrars may qualify for Fellowship status.
Fellows are then given Commonwealth accreditation under the Health Insurance Act to be recognised as providers of professional attention, for the purposes of health insurance rebates.
Prescribing & Referral Rights
There is considerable variation between state laws regarding the prescribing rights of Australian podiatrists.
While all registered podiatrists in each state or territory are able to utilize local anaesthesia for minor surgical techniques, some states allow suitably qualified podiatrists further privileges.
Recent legislative changes, which are expected to come into effect soon, will allow registered podiatrists and podiatric surgeons in Victoria graduates to prescribe relevant schedule 4 poisons.
In other states, such as Western Australia and South Australia, podiatrists with Masters Degree in Podiatry, and extensive training in pharmacology are authorised to prescribe S4 poisons.
In Queensland, Fellows of the Australasian College of Podiatric Surgeons are authorised to prescribe a range of Schedule 4 and one Schedule 8 drug for the treatment of podiatric conditions.
All podiatrists may refer patients for Medicare rebatable plain x-rays of the foot, leg, knee and femur, as well as ultrasound examination of soft tissue conditions of the foot.
Podiatrists may refer patients for other radiology investigations such as CT, MRI or bone scans, however Medicare rebates do not currently exist for these examinations.
Similarly, podiatrists may refer patients when needed to specialist medical practitioners, or for pathology testing, however similar exclusions in the Medicare Benefits Schedule prevent rebates being available to patients for these referrals.
Canada
In some parts of Canada the situation is legislatively stratified between the U.S. and British systems. For instance, in some provinces like British Columbia and Alberta, the standards are the same Doctor of Podiatric Medicine (DPM) level as in the United States. Quebec, too, has recently changed to the DPM level of training.
Also in Quebec, in 2004, Université du Québec à Trois-Rivières started the first program of Podiatric Medicine in Canada. In the prairie provinces, the standard has been based on the British model of chiropody.
Recognising this fact, in the province of Ontario, chiropodists and podiatrists are legislatively distinct occupational designations. Ontario chiropodists have a narrower scope of permitted practice than Ontario podiatrists (i.e., limitations on surgical practice).
New Zealand
Chiropody became a registered profession in New Zealand in 1969 with the requirement that all applicants take a recognized three-year course oftraining.
Soon after the professional title was changed from Chiropody to Podiatry and The New Zealand School of Podiatry was established in 1970 at Petone under the direction of John Gallocher.
Later the school moved to the Central Institute of Technology, Upper Hutt, Wellington. In 1976 the profession gained the legal right to use a local anaesthetic and began to introduce minor surgical ingrown toenail procedures as part of the scope of practice.
New Zealand podiatrists were granted the right of direct referral to radiologists for X-rays in 1984.
Acknowledgement of podiatric expertise marked improved services to patients and eventually in 1989 suitably trained podiatrists were able to become licensed to take X-rays within their own practice.
Diagnostic radiographic training is incorporated into the degree syllabus and on successful completion of the course, graduates register with the New Zealand National Radiation Laboratory.
In 1986, the profession undertook a needs analysis in conjunction with the Central Institute of Technology to identify competencies for podiatry in 2000. A Bachelor of Health Science was introduced in 1993.
United Kingdom
A podiatrist is qualified by their education and training to diagnose and treat conditions affecting the foot, ankle, and related structures of the leg.
Podiatrists are uniquely qualified among medical and health professionals to treat the foot and ankle based on their education, training and experience.
The scope of practice of UK podiatrists on registration after their degree in podiatric medicine includes the use and supply of some prescription only medicines, injection therapy and non-invasive surgery e.g. performing partial or total nail resection and removal, with chemical destruction of the tissues.
In a similar way to podiatrists in Australasia, UK podiatrists may continue their studies and qualify as podiatric surgeons. This training programme has developed over the last 30 years including development of standards in co-operation with the Scottish Royal Surgical Colleges.
The training requires a number of years study at postgraduate level including a Masters degree in the Principles of Podiatric Surgery, then a year as a pre-surgical trainee working within a podiatric surgical team, at least 2 years as a surgical trainee working to complete parts C and D of the surgical training and complete pre-Fellowship surgical training.
Following this, and having successfully passed a practical surgical assessment, a Podiatric surgeon will work at a specialist registrar (SpR) level for a minimum of three years under a Consultant Podiatric Surgeon.
This SpR period must be satisfactorily completed before being eligible to apply for a Consultant National Health Service (NHS) post.
These posts are subject to an appointments panel including an assessor from the Faculty of Surgery of the College of Podiatrists (an existing consultant podiatric surgeon).
Only if successfully appointed to such an NHS post may he/she then be able to use the title Consultant Podiatric Surgeon.
Podiatric surgery in the UK is not a recent development. The First UK training in podiatric surgery developed over 30 years ago in North London.
The original podiatric surgery faculty invited over by UK podiatric surgeons who had trained with them in the USA were leading US podiatric surgeons including; E Dalton McGlamry, Tildern Sockaloff, Guido LaPorta and later Lowell Scott Weil.
The First specific podiatric surgery in the NHS was provided via Shropshire Health Authority in 1983 and shortly after in the adjacent English county of Herefordshire.
The first specific podiatric surgery service was approved by Herefordshire Health Authority in 1986.
Subsequently these NHS services developed with Consultant Podiatric Surgeons being appointed to lead these growing services. The First dedicated NHS Podiatric Day surgery Unit was officially opened in Hereford in 1993.
There are now a number of NHS dedicated NHS Podiatric Day surgery Units and many NHS Trusts providing podiatric surgery.
A podiatric resident performs surgery on a patient who sustained trauma to the foot.
Podiatric surgeons specialise in invasive foot surgery. The scope of practice is defined as “surgery of the foot and associated structures”.
The majority of work reflects the frequency of foot pathology presenting in the UK, most commonly digital and forefoot surgery, as well as mid foot and rearfoot surgery including triple arthrodeses, ankle stabilisations and Achilles tendon lengthenings/repairs.
At present these surgeries are not carried out by all Podiatric Surgeons.
In the UK, individuals may not use the title “chiropodist” or “podiatrist” unless they are registrants of the Health Professions Council (HPC).
They are protected titles and their use by non-registrants is unlawful.[7] This protection extends to titles including the adjectival forms e.g. “podiatric surgeon” or “chiropody practitioner”.
Such registration is normally only granted to those holding a specialised Bachelors degree or Diploma in podiatry from one of the 13 recognised schools of podiatry in the UK.
The nomenclature surrounding the job titles of podiatric surgeons has been the source of some criticism from some constituencies within the medical community (in particular orthopaedics).
The stated concern underlying the criticism is that podiatric surgeons are not medically qualified or regulated by the Royal Surgical Colleges and may be misleading lay-people into believing that their title ‘podiatric surgeon’ implies that they are medically qualified and regulated by the Royal Surgical Colleges.
[8] This issue has been debated several times over the last 30 years despite the fact that all podiatric surgeons provide clear information to their patients regarding their training and qualifications as part of the process of informed consent.
Despite this much co-operation exists and in many areas podiatric surgeons and orthopaedic surgeons work closely together for the greatest benefit of patients, in multidisciplinary teams while respecting each others’ professional independence.
Appropriately qualified podiatrists are licensed to access and supply a limited range of POMs including antibiotics, analgesics, and steroids for injection.
Professional bodies recognised by the Health Professions Council are : The Society of Chiropodists and Podiatrists, The Institute of Chiropodists and Podiatrists, The British Chiropody and Podiatry Association and The Alliance of Private Sector Chiropody and Podiatry Practitioners.
Foot Health Practitioners: Since the 2005 statutory regulation/registration of the Chiropody/podiatry sector by the Health Professions Council there has been an increase in the number of former practitioners (of private sector chiropody) not being allowed to use their former title – (Chiropodist/Podiatrist) – as a higher degree (or the alternative diploma) in podiatric medicine etc became the required standard for statutory registration.
However this difficulty has now been addressed & former practitioners of Chiropody in the UK now use the newly established title of Foot Health Practitioner.
These practitioners provide many of the same treatments as private sector chiropodists & will refer clients who require more advanced treatments to a Chiropodist/Podiatrist.
Clients who have a condition not directly related to the health of the foot, but which was spotted by the Foot Health Practitioner will be immediately referred to a medical doctor,nurse practitioner etc for examination (this can be the case especially with elderly clients).
It should be noted that it is not only former chiropodists/podiatrists who use the title of Foot Health Practitioner.
There are now courses available from well established private training colleges throughout the UK allowing individuals with little or no health care experience to train to become a qualified FHP.
Appropriately trained foot Health Practitioners can become associate members of the following Health Professions Council recognised professional Podiatry/Chiropody bodies:
The Institute of Chiropodists and Podiatrists & The Alliance of Private Sector Chiropody and Podiatry Practitioners as well as other professional organizations that are not recognised by the HPC.
There is currently no statutory registration for practitioners in the private foot health sector – much like the lack of regulation of Chiropody/Podiatry prior to 2005.
United States
In the United States, podiatric medicine and surgery is practiced by a licensed Doctor of Podiatric Medicine (DPM). Education consists of a professional doctoral degree which is a four-year program followed by a two or three year residency.
This training follows a four-year undergraduate college degree. The first year of podiatry school is somewhat similar to training that physicians (either medical doctors or osteopathic doctors) receive, but with a limited scope on foot, ankle, and lower extremity problems.
Being classified as a second entry degree, in order to be considered for admission an applicant must first complete a minimum of 90 semester hours at the university level and/or complete a bachelor’s degree. In addition, potential students are required to take the Medical College Admission Test (MCAT).
The DPM degree itself takes a minimum of four years to complete. Thus there are five professions in the United States that allow for independent diagnosis and surgical treatment:
Doctor of veterinary medicine (DVM), doctors of medicine or osteopathic medicine (MD or DO), podiatric medicine (DPM), dental medicine (DDS and DMD), and optometric medicine (OD).
A podiatry student examines the adduction angle of the hallux.
The four-year podiatry school is followed by a residency, which is hands-on post-doctoral training. There are two standard residencies named Podiatric Medicine and Surgery 24 or 36 (PM&S 24 or PM&S 36).
These represent the two- or three-year residency training. Podiatric residents rotate through all main areas of medicine such as emergency, pediatric, internal medicine, and general surgery and of course podiatry — both clinic and surgical. During these rotations, attending podiatrists train the resident physicians in medicine and surgery.
Podiatric Foot and Ankle Surgeons certified by the American Board of Podiatric Surgery (ABPS) have successfully completed an intense board certification process comparable to that undertaken by individual MD and DO specialties.
Certification by the ABPS involves written, oral, and computer-based patient simulation questions, in addition to submission of surgical case logs.
Prerequisites for board qualification in Foot and Reconstructive Rearfoot/Ankle Surgery require successful completion of a three-year podiatric surgical program and passing a written examination.
ABPS board certification in Foot Surgery is a prerequisite for board certification in Reconstructive Rearfoot/Ankle Surgery.
A candidate must pass both the written, oral, and computer-based patient simulation questions in Foot Surgery as well as the written, oral, and computer-based patient simulation questions in Reconstructive Rearfoot/Ankle Surgery.
In addition, ABPS requires submission of 65 cases for certification in Foot Surgery and an additional 30 cases for certification in Reconstructive Rearfoot/Ankle Surgery, for a total of 95 cases.
ABPS requires four years of post-DPM degree clinical experience before taking the certification examination. Additionally, diplomats must recertify every 10 years to maintain their board-certified status, although some members who were certified prior to 1991 undergo a “self-test” examination, essentially circumventing taking the written exam all others must take in order to become re-certified.
In the United States, the previous titles used for the Doctor of Podiatric Medicine (DPM) degree were Doctor of Surgical Chiropody (DSC) and Doctor of Podiatry (PodD). Podiatry in the US currently encompasses a broader spectrum of practice than it used to.
Podiatrists can now perform medical and surgical procedures in all 50 states, though the specific scope of practice varies slightly in each state.
Early Educational Developments
William Scholl founded the Illinois College of Chiropody and Orthopaedics in 1912. Scholl was a Medical Doctor (MD) who felt the need to focus more on footcare.
Just prior to Scholl founding a Chiropody college in Illinois, other innovators and individuals around the United States were founding other institutions of learning for foot care.
Among these was M.J. Lewi, MD, who founded what is now the oldest and largest college of podiatric medicine located in New York City.
His institution later became the M.J. Lewi School of Podiatric Medicine and ultimately became the New York College of Podiatric Medicine.
The New York College of Podiatric Medicine notes that by 1911 the New York School of Chiropody had been created, dedicated to educating and training chiropodists.
Maurice J. Lewi, a physician and educator, then serving as Secretary to the New York State Board of Examiners, was named the first president of the school.
Lewi assisted in developing the first legislation governing the practice of chiropody. He also developed the curricula and training programs for the first course of study at the school.
Lewi was the first to suggest that the term “chiropody” be changed to “podiatry”, since the term “chiropody” was considered by some to be etymologically incorrect.
Some years later, the term “podiatry” was adopted by all other colleges of podiatric medicine and by the National Association of Chiropodists (NAC), now known as the American Podiatric Medical Association.
Podiatry was considered an adjunctive branch of medicine until Lowell Scott Weil, made contributions to the field which changed the course of the profession forever.
Considered the first true surgeon in the field of podiatry, Lowell Weil advanced the profession immensely by innovating surgical techniques in the foot and ankle.
The Weil osteotomy was named in his honor by legendary French Orthopedist Samuel Barouk. He continues to practice today in his 47th year in practice. As a result of his great success, he is often assaulted by members of his own profession who resent his meteoric rise and wealth.
Practice Characteristics
While the majority of podiatric physicians are in solo practice, there has been a movement toward larger group practices as well as the use of podiatrists in multi-specialty groups including orthopedic groups, treating diabetes, or in multi-specialty orthopedic surgical groups.
Some podiatrists work within clinic practices such as the Indian Health System (IHS), the Rural Health Centers (RHC) and Community Health Center (FQHC) systems established by the US government to provide services to under-insured and non-insured patients as well as within the United States Department of Veterans Affairs providing care to veterans of military service.
Scope Of Practice
The differences in podiatric medical and surgical practice are determined by state law. Each state allows or limits the practice of podiatric medicine to the foot. Some states allow other types of surgery.[citation needed] This may include surgery above the ankle and leg in 44 states. Most states require completion of a residency or a post-graduate training to practice.
Most podiatric surgeons work in surgery centers or hospitals performing both medical and surgical treatments for patients. As in many other specialties, some podiatrists work in nursing homes and some perform house calls for patients. Podiatric patients range from newborns and infants to the geriatric.
Surgical Practice
Within the scope of practice, podiatrists are one of two types of experts on foot and ankle care (the other type are orthopedic surgeons, a type of medical doctor). Some podiatrists have primarily surgical practices. Some specialists complete additional fellowship training in reconstruction of the foot and ankle.
Many podiatric surgeons specialize in minimally invasive percutaneous surgery. Most podiatrists utilize medical, orthopedic, biomechanical and surgical practices. Surgical podiatric principles rest on a base of orthopedic and kinesthetic knowledge.
United States
Within the United States medical and surgical care of the foot and ankle is mainly provided by two groups of physicians: Podiatrists (DPM) and Orthopedists (MDs or DOs).
Podiatrists who are certified in Foot and Ankle Surgery or certified in Foot Surgery and certified in Reconstructive Rearfoot/Ankle Surgery by the ABPS are specifically trained to diagnose and perform complex surgical treatments of the foot and ankle.
They are an integral part of the health care team, and combined with all other podiatric physicians, currently treat the majority of foot-related medical issues in the U.S. Orthopedists are the second largest providers of foot-related medical care.
Each ABPS board-certified Podiatric Foot and Ankle Surgeon has:
* Completed four years of Podiatric Medical School. The Podiatric Medical School curriculum covers basic and clinical sciences, including, but not limited to: general anatomy, pathology, biochemistry, pharmacology, general medicine, surgery, pediatrics, behavioral sciences, and ethics. Unlike MD and DO medical schools, the Podiatric Medical School curriculum also provides intensive foot and ankle “specialty” specific education beginning in the first year.
* Completed a post-graduate Podiatric Medicine and Surgery (PM&S) Residency (PM&S-24 or PM&S-36). While current Podiatric Residency models range from two to three years, the majority of graduates complete three years of podiatric surgical training and some continue on to do fellowships.
You can find much more information on living a holistic lifestyle in these free magazines and on our YouTube channel.
Information courtesy of Wikipedia